CAR+ T-cell lymphoma linked to cilta-cel therapy in myeloma
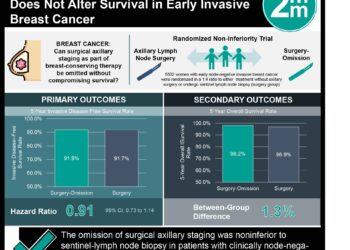
1. This study describes two cases of malignant monoclonal T-cell lymphoproliferation following ciltacabtagene autoleucel (cilta-cel) Chimeric Antigen Receptor T-cell (CAR T-cell) therapy for relapsed/refractory multiple myeloma in the CARTITUDE-4 trial.
2. The CAR transgene was detected in malignant T cells, suggesting integration into preexisting mutated T cells, with further genomic alterations contributing to lymphomagenesis.
Evidence Rating Level: 4 (Below Average)
Study Rundown: CAR T-cell therapy is a method of engineering receptor proteins to allow T cells to target cancer-specific antigens. These therapies are particularly promising in the realm of hematologic malignancies. Recently, anti-B-cell maturation antigen therapies have been explored for the treatment of multiple myeloma. Cilta-cell is one of these and is specifically produced using lentiviral transduction. This study presents two cases of CAR T-cell therapy-associated peripheral T-cell lymphoma (PTCL) arising after cilta-cel infusion. The genomic analysis suggests an interplay of preexisting TET2 mutations, insertional mutagenesis, viral infections, and previous myeloma treatments as potential contributors. Despite the rarity of such cases, the findings highlight the need for long-term monitoring of CAR T-cell therapy recipients. Strengths include comprehensive genomic characterization, while limitations include the inability to determine a direct causal link between CAR insertion and lymphoma development and the small sample size.
Click to read the study in NEJM
Click to read an accompanying editorial in NEJM
In-Depth [case series]: This case series describes two patients from the CARTITUDE-4 trial who developed CAR+ T-cell lymphoma following treatment with cilta-cel, an anti-B cell maturation antigen CAR T-cell therapy for relapsed or refractory multiple myeloma. The study investigates the genomic and clinical features of these rare malignancies and possible mechanisms underlying the development of T-cell lymphoproliferative neoplasms. Patient 1, a 51-year-old man, developed a nasofacial skin lesion five months after cilta-cel infusion. The lesion biopsy confirmed a PTCL expressing the CAR transgene. Whole-genome sequencing identified a TET2 mutation, which had been present at low levels before CAR T-cell therapy but expanded significantly afterward. Additional genomic findings included a germline JAK3 mutation and CAR integration into the PBX2 gene, though no clear oncogenic dysregulation was observed. The patient initially responded to chemotherapy but relapsed multiple times, requiring allogeneic stem-cell transplantation and experimental therapies. Patient 2, a 54-year-old woman, presented with multiple skin lesions and systemic lymphadenopathy 16 months post-infusion. The disease exhibited a monoclonal CD4–CD8– T-cell phenotype, and the CAR transgene had integrated into the ARID1A gene, a tumour suppressor frequently altered in cancers. Unlike Patient 1, she initially experienced spontaneous lesion regression, followed by widespread disease progression. She underwent haploidentical allogeneic stem-cell transplantation and, at the last follow-up, was in complete remission with no detectable circulating CAR+ T cells. The findings suggest that preexisting TET2-mutated T cells, coupled with lentiviral CAR transgene integration and possible immune stimulation, may have contributed to lymphomagenesis. While causality remains uncertain, these cases raise important safety considerations for CAR T-cell therapy.
Image: PD
©2025 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.